Mention the word cannabis and the confusion starts; legal or illegal, nutraceutical or medicinal product, psychoactive or non-psychoactive, clinically significant or not. At the same time, the cannabis industry is booming with conservative global estimates of $32 billion USD by 2022, which would be an approximate increase of > 300%. Currently, the industry is focused on exploiting the benefits of medicinal cannabis and the purification of cannabinoids for use in medical products. In this blog, you will find out more about the regulations and compliance standards regarding medicinal cannabis and what to expect of it in the near future.
- DEFINITIONS
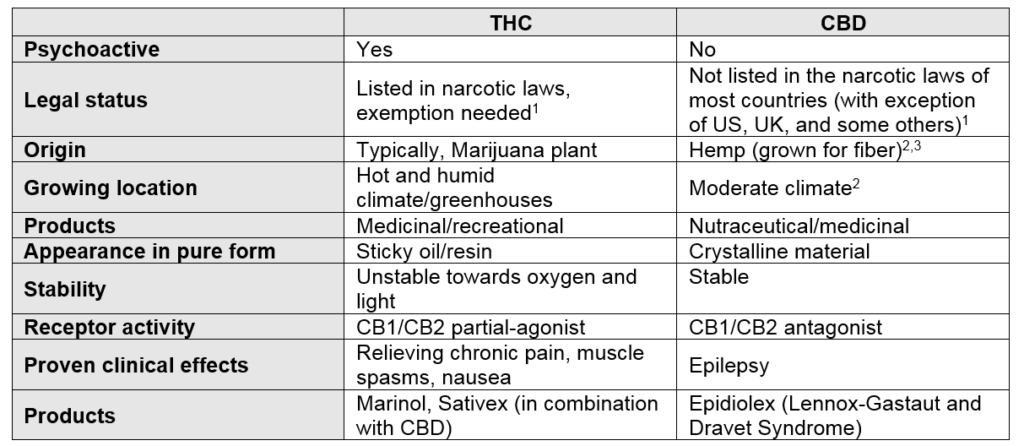
The first thing to set straight is the name cannabis. This is not a specific type of plant or product but more an all-encompassing term of a number of plants, materials, and products. While there are over a hundred known active substances (cannabinoids) in cannabis with slightly different chemical structures, the two most common are THC and CBD and are representative for the majority of endeavors in cannabinoid product development. THC and CBD are quite different from one another and in the table below you can see a comparison.
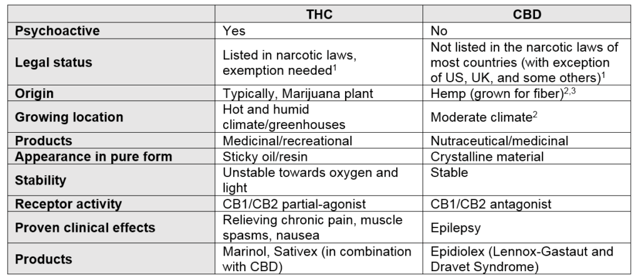 1 Please check the legal status in your country or state prior to development of cannabis products
1 Please check the legal status in your country or state prior to development of cannabis products
2 Specially bred CBD-containing plants are often grown in greenhouses and are mainly intended for medicinal products
3 If hemp is grown to isolate CBD, an exemption from the narcotics law is required in most countries
- REGULATIONS
Currently, there are 47 countries, mainly in Europe and the Americas, where medicinal cannabis is either legal or legal with certain restrictions. It is usually prescribed by a physician and provided by pharmacies. Pharmacies obtain their packaged product from wholesalers and those from growers of cannabis plants. Both the growers and the distributors require licenses from state or municipal offices to be allowed to work with this plant material. To obtain such a license most regulatory agencies require demonstration of:
- protective measures to prevent unaccounted cannabis material
- specific processes for handling of the material
- controls and accountability of growing process
- importing
- re-packing
- storage controls
- distribution
- R&D-activities
Currently there are numerous producers that have been successful in obtaining the proper licensing; however, it can be complicated to produce / distribute in multiple at the same time because each country has its own set of regulations.
- QUALITY STANDARDS
When producing, storing or distributing medicinal cannabis, Health Authorities may require a product to comply with the standards described in the country’s Good Manufacturing Practice requirements, e.g. EU countries. This is managed by clearly defining specifications for possible quality risk factors like:
- content
- moisture
- foreign matter
- microbiology
Interestingly, GMPs are not required for planting or seeding of cannabis plants. Instead, this typically requires Good Agricultural Practice, which secures a constant quality of the plant material and is often done in a secured greenhouse). GMP usually starts at harvest of plant buds.
- EXTRACT OR PURIFIED SUBSTANCE?
Currently, the cannabis industry’s focus is changing from plant material such as terpene oils to the extraction and purification of the cannabinoids. While the plant material does exert a beneficial effect and dried buds are easy to obtain and use (e.g. teas, smoking, etc.), it comes as no surprise that standardizing the use of cannabis to secure constant dosing for patients is key and certainly worthwhile to investigate more advanced ways of delivering cannabinoids. For instance, by presenting an extract or purified THC / CBD to patients you increase your control over the contents and dosing becomes more accurate, opening possibilities to investigate treatment efficacy in clinical trials. A number of companies are already using purified THC and CBD (essentially pure active substances) in clinical studies aimed at obtaining marketing authorization.
Example: The drug product Sativex is manufactured by extracting the cannabinoids from the entire cannabis plant and formulating it as a spray. GW Pharma obtained a marketing authorization for Sativex in 25 countries outside the US for treatment of spasticity.
The authorization of Sativex is remarkable because the extracts from the cannabis plant still contain a large number of other cannabinoids as well as terpenes. Although we assume the activity in Sativex is from the THC and CBD, it is not clear which components are specifically responsible for the therapeutic effect.
- FORMULATION
Whether extracts or purified cannabinoids are used, there is several possibilities to administer these active substances to patients; each with their own pros and cons. When working with medicinal cannabis, it is important to start with the patient in mind and define requirements that will treat a patient in the most comfortable / appropriate way possible.
Some of the formulations:
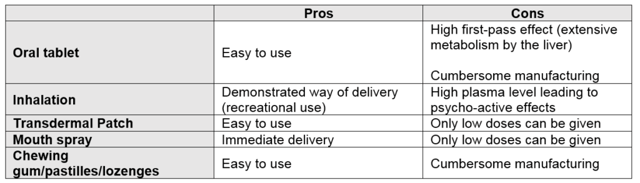

- STABILITY
One aspect that needs to be considered when extracting and purifying THC is its stability, or rather its instability. Unlike CBD, THC is vulnerable to oxygen, light, and possibly moisture, and it is readily decomposed by radical oxidation. This means standard formulation techniques may not be sufficient to provide a stable drug product and instead requires encapsulation techniques. Methods have been developed to protect the THC by encapsulation into a polymeric or a liposome matrix. Surprisingly, the dissolution in aqueous ethanol mixture also exerts a stabilizing effect as demonstrated by the Sativex spray developed by GW Pharma.
- CLINICAL STUDIES
As previously stated, a number of treatments have been approved world-wide by Health Authorities. These are mainly in the area of pain reduction, emesis, nausea and symptom reduction in MS-patients. It is known that cannabinoids act on a multitude of different receptors in the body, either as agonists or antagonists, and could potentially interfere with disease mechanisms. Therefore, cannabinoids are thought to have the potential to treat or cure diseases such as cancer (see e.g. the excellent review paper of Massi et al. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3579246/ )
FUTURE
So, why haven’t we found more cures to date? Is it possible that the multi-compound containing cannabis material has hampered the progression of the use of cannabinoids in approved treatments? As indicated before, cannabis materials are challenging to define and characterize due to the number of cannabinoids and terpenes, along with the multitude of administration routes. Therefore, claims using medicinal cannabis are difficult to be substantiated with clinical evidence. With THC and CBD now readily available as GMP-material, the scientific community is more suitably equipped to perform clinical studies. Hopefully resulting in approved drug products that treat patients safely and effectively.